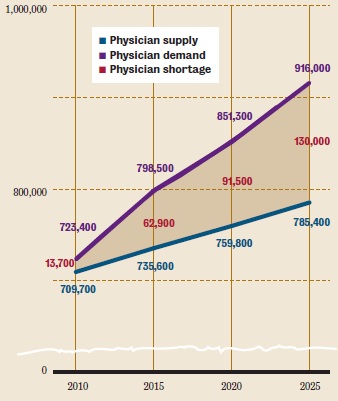
Source: AAMC Center for Workforce Studies, June 2010 Analysis
Healthcare in the United States is continuously changing. Over the last few years, the rate of change has been accelerating. With the passing of the Affordable Care Act (ACA), the stage has been set for even more change that will occur at an even faster pace. The recent ruling by the Supreme Court, which stated that the individual mandate of the ACA is constitutional, has taken the people of the United States closer to universal health insurance coverage. This is an exciting time for both patients and their physicians.
The ACA is a noble and praise-worth endeavor, but it has failed to address an impending disaster in the American healthcare system. That impending disaster is the physician shortage, which was well on its way even before the ACA was passed into law. Based upon estimated projections, the United States will be short staffed by about 91,500 physicians by the year 2020, and by 130,000 by the year 2025. In 2014, the ACA will introduce 32 million newly insured patients into the healthcare system of the United States. This will undoubtedly cause the physician shortage to become even worse.
How can we solve this very important problem?
Several new medical schools have been established throughout the United States. In addition, the already existent medical schools have expanded their class sizes in order to train even more physicians. This combined effort in estimated to produce 7,000 additional physicians each year. Despite this, there will still be a physician shortage.
The president and CEO of the Association of American Medical Colleges, Dr. Darrell Kirch, expressed his concern for this subject on March 16, 2012 during residency match day. He wrote, “To help avert the doctor shortage, the nation’s medical schools have been expanding enrollment since 2006 and are now on track to educate 30 percent more M.D.’s by 2017. Teaching hospitals also have entirely self-funded the training of thousands of additional doctors since 2000. But these increases are not enough to avert the expected shortage of 90,000 physicians by 2020”. In addition, he wrote, “With 32 million Americans set to enter the health care system in 2014, and a growing and aging population who will live longer and need more medical care, the nation’s medical schools and teaching hospitals are doing all they can to address the shortage”.
In addition to educating more physicians, our medical education system needs to make more graduate medical education (GME) positions available. The Balance Budget Act of 1997 capped the number of Medicare funded GME positions to about 100,000. Our politicians must increase this limit on GME positions in order to provide more adequately trained physicians. In addition, there should be incentives for medical students to enter into the primary care fields, which are expected to be in highest demand.
I am privileged to have a front row seat and witness the changes that are about to take place in our nation’s healthcare system. There are many times when I feel overworked and pressured to see more patients in less time. With the growing physician shortage, the pressure to work more efficiently will become even greater. Most physicians will not mind working harder, but I believe that all physicians will not accept a compromise in patient care that will most likely occur if the current physician shortage trend continues. In the end, it is the patient that will suffer the consequences of a physician shortage. It takes over a decade to train a physician, and we will not see an increase in the physician numbers for some time. We must act now to avert this future disaster.
Reference:
“Physician Shortages to Worsen without Increases in Residency Training” Association of American Medical Colleges Center for Workforce Studies, June 2010 Analysis







 DrSamGirgis.com is a blog about medicine, nutrition, health, wellness, and breaking medical news. At DrSamGirgis.com, the goal is to provide a forum for discussion on health and wellness topics and to provide the latest medical research findings and breaking medical news commentary.
DrSamGirgis.com is a blog about medicine, nutrition, health, wellness, and breaking medical news. At DrSamGirgis.com, the goal is to provide a forum for discussion on health and wellness topics and to provide the latest medical research findings and breaking medical news commentary.
{ 0 comments… add one now }